The Impact of Nursing Resources on Sepsis Outcomes
SUMMARY
-
Nurses play an important role in effective sepsis identification and management.
- The level of nursing resources varies across hospitals, with better resourced hospitals demonstrating improved clinical and economic sepsis outcomes.
- System level attention to nursing resource levels in sepsis should be evaluated.
BACKGROUND
Nurses have a significant role is sepsis management protocols. Nursing led screening, initial assessment of suspected sepsis and protocol implementation have demonstrated improved sepsis bundle compliance. Despite this data, additional studies are needed to determine the most effective way to achieve sepsis endpoint targets.
Nursing staffing ratios and skill mix (i.e. nursing resources) vary across hospitals. Recently Lasater et al., evaluated how different nursing resource levels impact the clinical outcome and costs (via standardized national pricing) of sepsis.
REVIEW
- Matched cohort Medicare patients from 306 acute care hospitals in 4 states were included from January 1, 2013 to September 30, 2015.
o Hospitals were categorized by size, teaching status and technology capabilities.
- Patients were closely matched on over 60 comorbidities and demographic characteristics.
- In addition to sepsis, heart failure, pneumonia, stroke and acute myocardial infarction were evaluated.
- Hospitals were segmented to those with better or worse nursing resourced hospitals.
o Nursing resources consisted of:
-
- Patient to Nursing Staffing: # patients per direct care of RN
- Skill Mix: % of RN to all nursing staff (RN, licensed practical nurses and unlicensed assistants).
- Education: % bachelor’s degree in Nursing (BSN) or higher
- Nurse Work Environment: 31 item Practice Environment Scale of the Nurse Work Index Score
OUTCOMES
- There were approximately 3 times as many worse nursing resourced hospitals than better resourced hospitals.
- Each of the 4 nursing resource dimensions were statistically superior in better resourced hospitals compared to worse nursing resourced hospitals.
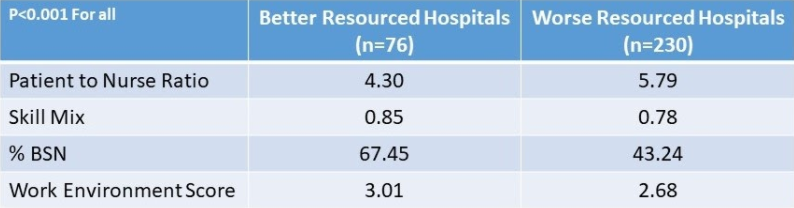
TABLE 1: Comparison of Better and Worse Nursing Resourced Hospitals
- 25,446 match sepsis paired were identified
- Lower sepsis mortality, sepsis readmission, ICU admissions, length of stay occurred in better nursing resourced hospitals as compared to worse resourced hospitals, with all variables being statistically significant.
- Total costs as well as cost after adjusting for higher costs associated with better staffing and skill mix were significantly lower with better resourced hospitals.
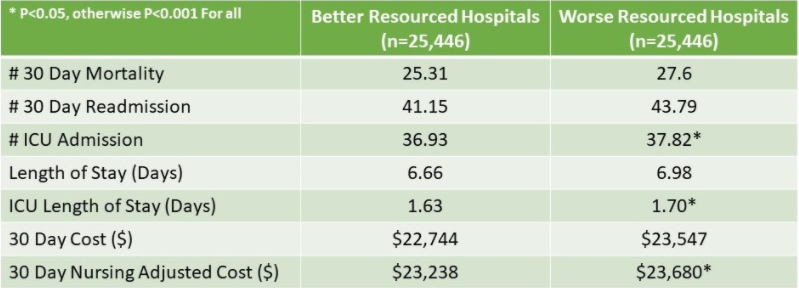
TABLE 1: Comparison of Better and Worse Nursing Resourced Hospitals
CONCLUSIONS
- Although limited to Medicare patients, sepsis outcomes and cost of care was superior in hospitals with better nursing resources.
- System level attention to nursing resources may be an important consideration in improving sepsis outcomes.
To receive articles like these in your Inbox, you can subscribe to Sepsis Program Optimization Insights.
Erkan Hassan is the Co-Founder & Chief Clinical Officer of Sepsis Program Optimization where he designs & oversees the implementation of solutions to optimize sepsis programs.
To discuss your organization’s Barriers of Effective Sepsis Care, contact Erkan by phone (844) 4SEPSIS (844-473-7747), email (erkan@spo.icu), or video chat.





