Can Biomarkers Aid in Sepsis as a Diagnostic and Prognostic Tool?
One of the areas which has hampered our overall approach to sepsis is the lack of a gold standard for the diagnosis of sepsis. In addition, traditional culture methods are time-consuming and often times do not reveal a causative microorganism. Reliance of cultures may result in patients being under or over treated.
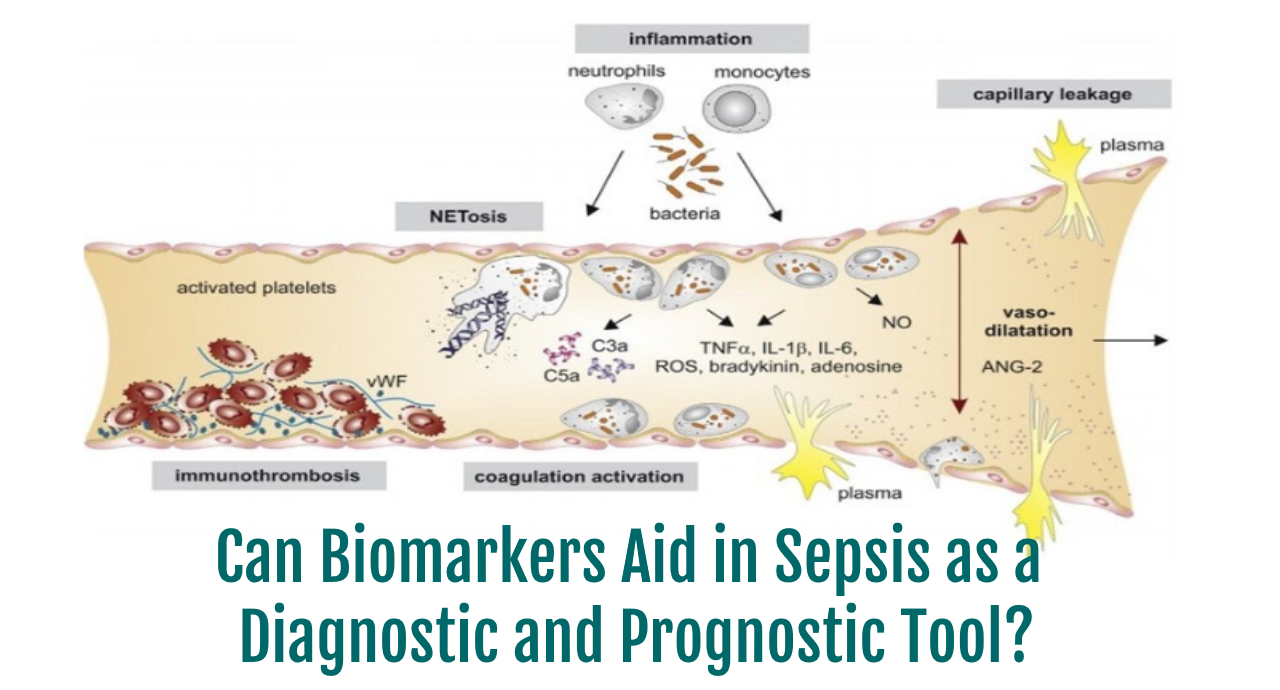
Improvements in sepsis should address identification prior to organ dysfunction requiring rapid diagnosis and onset of treatment. Sepsis is characterized by overwhelming systemic inflammation. Biomarkers which are significantly activated in the early stages of the infectious cascade may provide an easy and rapid source of insight and information.
Potential uses of biomarkers in sepsis would be to:
- Provide early identification of disease and severity
- Aid in clinical decision making regarding ICU requirements
Previously, numerous biomarkers have been evaluated in sepsis, but have not exhibited robust performance. These include:
- Interleukins (IL-) 1, 2, 4, 6, 8, 12
- Procalcitonin (PCT)
- Complement components – C3a, C5a
- C-reactive protein (CRP)
The activated immune response to sepsis results in:
- The release of pro-inflammatory and anti-inflammatory mediators
- Followed by a rise in levels of acute phase proteins
- Additionally, serum levels of glycoproteins on cell membranes
Although there are a large number of potential compounds, the items in the table have developed to the point of clinical comparisons.
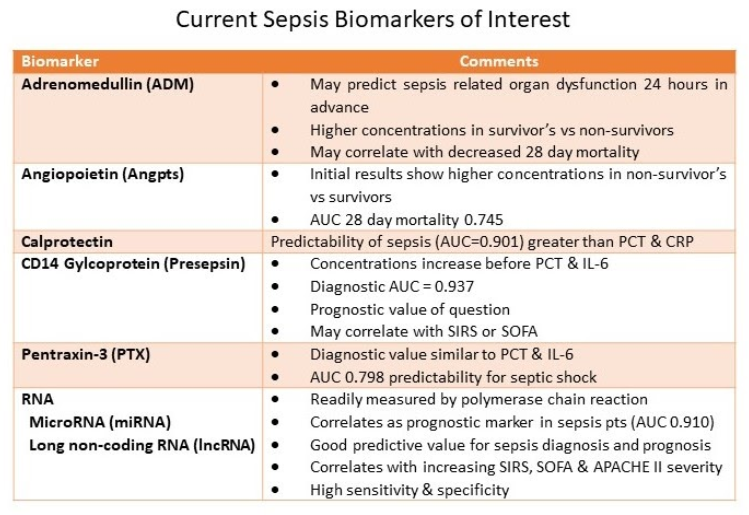
Conclusions:
Abnormalities in the immune response range from excessive inflammation to immunosuppression contribute to disease pathogenesis. Biomarkers may help overcome current limitations in predicting sepsis diagnosis and prognosis. Addressing immunologic gaps in the pre-sepsis phase, during sepsis, and post-sepsis phase will help to design superior diagnostic and treatment approaches.
To receive articles like these in your Inbox, you can subscribe to Sepsis Program Optimization Insights.
Erkan Hassan is the Co-Founder & Chief Clinical Officer of Sepsis Program Optimization where he designs & oversees the implementation of solutions to optimize sepsis programs.
To discuss your organization’s Barriers of Effective Sepsis Care, contact Erkan by phone (844) 4SEPSIS (844-473-7747), email (erkan@spo.icu), or video chat.